Learning and knowledge sharing are fundamental to the LHSS Project. We invite you to search LHSS knowledge products and resources for the latest approaches, insights, and learning in the field of integrated health systems strengthening.
To advance progress toward universal health coverage, agreed-upon health priorities need to be reflected in national plans and budgets. This blog offers key lessons for ministries of health seeking to make that happen.

This learning resource presents key learning from the activity literature review, learning exchange meetings, and TA workshops. This resource focuses particularly on stakeholder engagement and institutionalizing stronger links between national health priorities, sector plans and national budgets, which learning partners identified as their most pressing issues.
This document outlines LHSS’s strategy for supporting the strengthening and scale up of local capacity through country and core activities. Designed for use by LHSS staff and local partners, this strategy provides a framework and details on how to develop, implement, monitor, and evaluate sustainable health system strengthening activities. This strategy replaces the LHSS Scale Up of Local Capacity Strategy (2019).

Given the complexity of the causes and effects of the SDoH and the multitude of stakeholders and interventions needed, this publication introduces the Theory of Change (ToC) that can help those seeking to develop interventions to address and mitigate the effect of the SDoH on health.
This analysis establishes a baseline understanding of current cross-border health challenges and opportunities, and identifies organizational and technical capacity gaps to address within key stakeholders that are leading cross-border health initiatives.

In this webinar, we discuss promising practices for establishing a learning culture. Dr. Malangizo Mbewe, Acting Director, Quality Management Department, Ministry of Health and Population in Malawi, also shares his experience establishing systems to support continuous quality improvement.
While securing adequate funding to improve quality of care is a challenge for many countries, some have been successful implementing financial mechanisms to incentivize high-quality care delivery, reducing fraud, waste, and abuse.
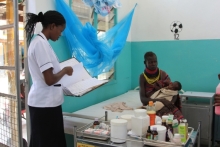
Representatives from Kenyatta Hospital share their experience engaging stakeholders, understanding the health and healthcare needs of the population, and translating those needs into a cohesive NQPS.
