Learning and knowledge sharing are fundamental to the LHSS Project. We invite you to search LHSS knowledge products and resources for the latest approaches, insights, and learning in the field of integrated health systems strengthening.

In a municipality where over 100,000 people had no access to basic health services, stakeholders joined together to open a primary health center that now serves thousands of households.
This learning brief captures LHSS’s experience in supporting municipal-level partners through the contracting process and distills emerging lessons to inspire other municipalities to pursue public-private partnerships as a vehicle for expanding access to urban PHC services.
This brief presents what LHSS has learned through applying a systems thinking approach to its support for HSCs’ advocacy efforts in expanding PHC services in urban Bangladesh.
New efforts will make health care more affordable for residents in 10 municipalities.

LHSS is supporting local government institutions in Bangladesh’s densely populated Rajshahi and Sylhet Divisions to expand access to primary health services and reduce out-of-pocket expenditures for low-income urban residents.
This brief highlights learnings from working with local government leaders of two city corporations and ten district-level municipalities from the Rajshahi and Sylhet divisions in Bangladesh.
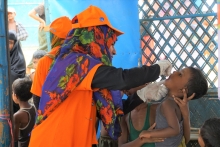
Both Ghana and Bangladesh have implemented health budget accountability mechanisms. Their experiences offer practical lessons that other countries can adapt to their own budget execution needs.
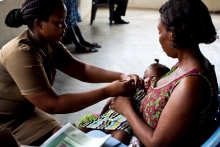
Late last year, health sector practitioners from eight countries met to tackle the issue head-on as participants in the Joint Learning Network Health Budget Execution Learning Exchange. They made meaningful progress.

By now, much has been written about the egregious global inequities in COVID-19 vaccine distribution. But less has been said about another inequity that holds serious implications for global health: the disparities in genomic sequencing capacities and capabilities worldwide.

Poor budget execution results in inefficiencies that undermine the ability of health agencies to improve access to needed health services and improve population health. Yet billions of dollars in unexecuted health budgets are returned to treasuries every year.

The events of the past 18 months underscore the importance of generally strong, equitable, and accessible health systems. COVID-19 is not the only threat we face, and as we prepare for the future it is critical that we begin to sufficiently invest in the foundational health system strengthening required to develop lasting resilience.

The proliferation of mobile telephones and advances in digital financial technology have created opportunities for faster progress towards achieving Universal Health Coverage.
