Learning and knowledge sharing are fundamental to the LHSS Project. We invite you to search LHSS knowledge products and resources for the latest approaches, insights, and learning in the field of integrated health systems strengthening.
To advance progress toward universal health coverage, agreed-upon health priorities need to be reflected in national plans and budgets. This blog offers key lessons for ministries of health seeking to make that happen.

Routine stakeholder engagement is critical to fair and inclusive national priority setting for health, but many countries face challenges in reaching key groups. This blog shares promising practices for bringing in key stakeholders and making sure the loudest voices aren’t the only ones heard.
For countries wanting to strengthen health budget execution, learning about promising approaches used by others is one thing but putting them into practice is another. This blog reveals how two countries, Lao PDR and Peru, adapted promising practices and began to implement them.

Ministries of health know that priority setting is important, but explicit priority-setting processes — processes that are inclusive, transparent, and informed by evidence — often are not institutionalized. This blog shares the promising practices being used in several countries.

How can countries make progress towards good health budget execution? In this latest blog in our budget execution series, ministry of health practitioners from eight countries offer lessons based on their own experiences and shared learning.

Through an LHSS-Joint Learning Network learning exchange, health practitioners from seven countries are sharing successful experiences and promising practices to institutionalize explicit national priority-setting processes for health. The goal? To help countries set equitable national health priorities and ensure that these priorities are reflected in national health plans and budgets.
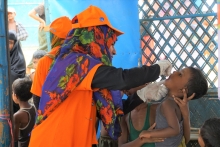
Both Ghana and Bangladesh have implemented health budget accountability mechanisms. Their experiences offer practical lessons that other countries can adapt to their own budget execution needs.
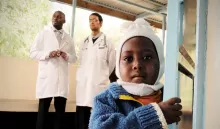
What do Lao PDR, Malaysia, and Kenya have in common? All three countries have strengthened their budget structures and processes to enable good health budget execution. Their experiences hold valuable lessons for others striving to increase budget execution and unlock significant resources for health.
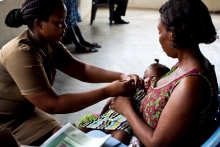
Late last year, health sector practitioners from eight countries met to tackle the issue head-on as participants in the Joint Learning Network Health Budget Execution Learning Exchange. They made meaningful progress.

By now, much has been written about the egregious global inequities in COVID-19 vaccine distribution. But less has been said about another inequity that holds serious implications for global health: the disparities in genomic sequencing capacities and capabilities worldwide.

She’s a big thinker, with an illustrious background. Midori de Habich was Peru’s minister of health and chair of the South American Council of Health from 2012-2014. She has served on various WHO working groups and missions and led USAID-funded projects in Peru. Now, she is applying her expertise in financial protection and population coverage to LHSS as the project’s technical director.

It is easy to fall back on the habit of using catchall terms like “vulnerable groups” to refer to many different people, but relying on these terms can have a harmful unintended consequence.

For countries facing a large influx of migrants, the best way to ensure that these new members of society have sustained access to essential health services is to have a long-term strategy – one that builds on existing health platforms.

In the Dominican Republic, the dual impact of large numbers of migrants and a health system overwhelmed by COVID-19 has meant that fewer health services are available for migrant women. LHSS is working to improve health protection for the country’s migrant women, most of whom come from Haiti.

Population movement of this magnitude places huge stress on health systems in receptor countries. How can health care for migrants be financed? How can health system capacity be expanded? And how can health sector policies and national migration policies be harmonized?
